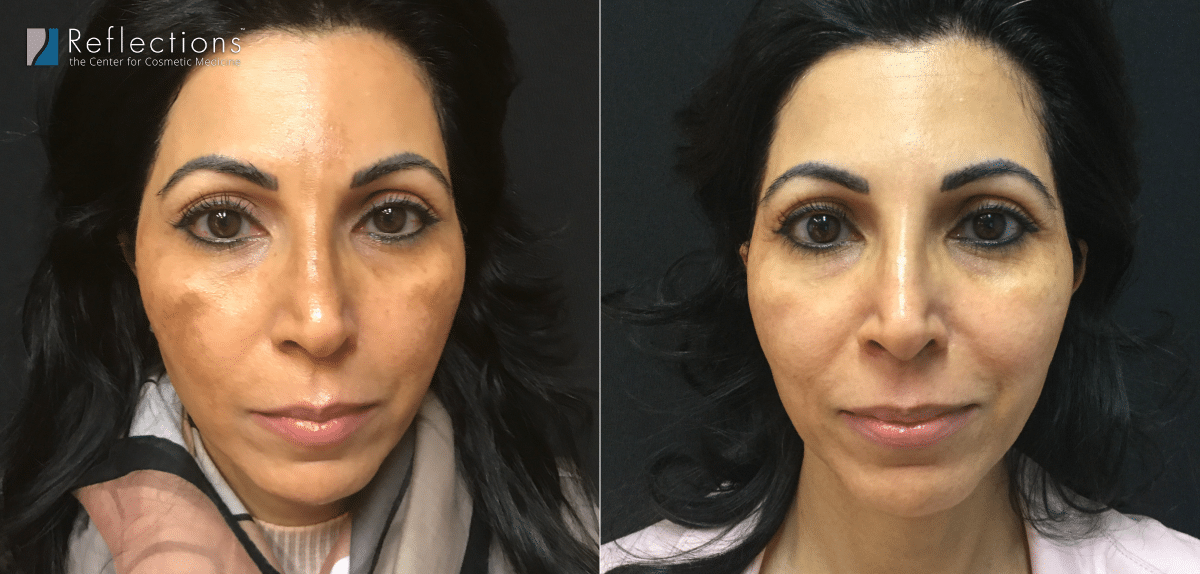
This is a new and promising treatment for melasma that’s been slowly gaining support for almost a decade now as the off-label use of this FDA-approved drug, and now has some really good science behind its use in adults with melasma.
Tranexamic Acid (often abbreviated as TXA or TA) is a synthesized amino acid that is used to treat moderate to severe melasma, especially in patients that have not had success with other treatments like lasers, skincare (sunscreen), and other prescription medication.
Tranexamic Acid Quick Facts
- New, Cutting-Edge Treatments for the Most Stubborn Melasma
- Oral Prescription Medication or Micro-Injections Procedure, TXA Restore
- Easily Paired with Laser Treatments
- Safe for All Skin Tones & Types
How Do You Use Tranexamic Acid to Clear Melasma?
Creams and serums that contain TXA aren’t effective because the molecule is too big to penetrate the skin and reach the deepest parts of the skin, where the drug can be effective at stopping pigmentation creation. Laying on top of the skin, TXA does you no good. Unfortunately, like with all new discoveries in cosmetic medicine, you often see skincare companies touting their formulas because they know the active ingredient has gained a reputation for working – but most of the time, it’s just a marketing tactic. And that’s certainly the case with Tranexamic Acid.
You will also see some medspas and practitioners microneedling the skin and applying tranexamic acid topically (rubbing into the skin through puncture channels) this method is problematic because the dosage is not precise: the channels close very quickly and at an uneven rate – and you never really know how deeply the product you’re rubbing in is penetrating, or how evenly it’s entering those channels.
Micro-Injected Tranexamic Acid: TXA Restore, Available Exclusively at Reflections

Historically, we’ve known that tranexamic acid placed within the skin is really the ideal – because it circumvents the systemic side effects, which can be significant with TXA – but it has been a struggle to find a way to get the TXA evenly deposited throughout the skin at the depths it works best.
It’s only been in the last year that we’ve developed a method of precisely depositing the TXA in uniform droplets at a uniform depth, and this is done through our own proprietary treatment, called TXA Restore.
This microneedling injection device has 3 important distinctions from traditional microneedling in that:
-
- the needles are depositing the TXA through hollow tips
- the amount of TXA being deposited is controlled through a precision injection tool
- the depth is also precisely controlled by the device, so we can be exact about where we have the drug delivered, and even layer it within the skin
This also means the treatment is much faster and more comfortable for the patient.
- Recovery & Downtime: None
- Numbing: Available
- Cost: Discuss at your free consultation
- Candidacy: Patients without sensitive skin
- Duration: Long-lasting
- Why We Love It: Deposit medication deep into the affected skin layers
Tranexamic Acid Pills (Prescription)

Most patients respond to the combination of oral tranexamic acid, topical hydroquinone, and either Q-switched Nd:Yag or Clear + Brilliant laser treatments within 3-4 weeks.
Normally a total of 3-4 laser treatments are provided approximately 2-4 weeks apart (Q-Switched Yag interval is 2-3 weeks apart and Clear and Brilliant interval is 3-4 weeks apart), while tranexamic acid pills will be prescribed for a period of 3-6 months, and topical skincare, while the individual products recommended may change over time, will be a lifetime commitment in order to best-manage melasma.
Oral tranexamic acid (TXA prescription pills) has been shown to be an effective way of managing melasma, to decrease the creation of new pigment – so that the effects of laser treatment and hydroquinone to remove existing pigment are long-lasting. However, this pill format means that the TXA is dispersed throughout the entire body, and TA will have some side effects, which make it not a good choice for every patient, especially in pill format, where the effects are much more widespread than in a topical or injected formula – but remember that the topical format of tranexamic acid is not going to be effective, since the molecules are too big to enter deep enough into the skin without being injected there.
- Recovery & Downtime: None
- Numbing: None
- Cost: Will depend on your health insurance policy’s prescription coverage
- Candidacy: Patients with severe melasma that isn’t well-treated with other prescriptions, skincare, and laser – this is the last resort.
- Duration: Long-lasting
- Why We Love It: Creates amazing results for people who just weren’t getting any or full results before.
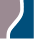


Why Choose Reflections Center for Tranexamic Acid for Melasma Treatment
Our Reflections team cares about our patients and we understand the struggles that many people go through to achieve healthy, beautiful skin. We now offer tranexamic acid in two different types of treatment for patients with melasma that has not responded to other forms of treatment. We’ve dedicated our time to research the newest and best treatments for our patients and many are loving the results they achieve from tranexemic acid!
We also understand that no two patients are the same, which is why our team takes the time to speak with our patients regarding medical history and aesthetic goals. We take this information and create a personalized treatment plan for each person for the best possible results.
Schedule Your Free Consultation
When you arrive for your free consultation with a Reflections physician, we will discuss your skin history and the treatments you have tried to resolve your melasma. Our goal is to help you find an effective treatment and we are happy to try a few different options until we find one that works.
Frequently Asked Questions About
Tranexamic Acid for Melasma
- How does tranexamic acid work for melasma?
Tranexamic Acid (TXA) is a particular version of the amino acid Lysine, which works within the skin to prevent melanocytes from fully forming new melanin. This is a harmless effect, but by inhibiting the skin from forming new melanin, we can stop the forming of new dark spots in patients with melasma.
- Does tranexamic acid lighten skin?
No, tranexamic acid prevents your skin from laying down new pigment (or darkening) for a short period of time. Generally, this 3-6 month application of this drug allows those with melasma to calm down the overactive melanocytes that are causing this skin disorder, and it’s often paired with laser treatments that remove the existing dark patches, to create skin that’s even with your natural complexion tone.
- Is tranexamic acid FDA-Approved for treatment of melasma?
No, tranexamic acid has not been FDA-approved for melasma specifically, but here’s why that doesn’t matter all that much.
TXA has been FDA-approved for patients with blood and clotting disorders. Well, as we have been using tranexamic acid to treat these patients since the early 1960s, several of them also suffered from melasma and reported this happy side effect of a clearer complexion.
Since the 1980s, several clinical studies have shown its safe and effective use in treating melasma (both in the US and internationally, on patients of all types) – but the pharmaceutical companies have decided not to (yet) pursue FDA approval (likely because each new FDA-approval costs several million dollars to go through the process, and because there is a good deal of drugs used off-label in the way tranexamic acid is for melasma, especially when the drug has a long history of safety and efficacy, as is in this case).
- How long can you take tranexamic acid for melasma?
It is common to prescribe Tranexamic acid for 3-6 months when used as a treatment for melasma.
- How long does tranexamic acid take to work for melasma?
In one study, comparing daily topical hydroquinone 2% versus intradermal injections of tranexamic acid performed monthly, the tranexamic acid showed much bigger results at the one-month mark2. However, you will need 3-6 months to see the full results from prescription-strength TXA, whether that’s injected or pill format.
- How effective is tranexamic acid for melasma?
When combined with a carefully chosen laser technology, appropriate for the skin type of the individual, tranexamic acid is very effective for melasma in either pill or micro-injected form. Topical tranexamic acid is less effective (remember that skincare strength is also far less potent).
- Is tranexamic acid safe for dark skin?
Oral tranexamic acid is safe for the treatment of melasma in skin of color, but one needs to be cautious when it is used in its injectable form due to the risk of causing pigment alteration.
- Is tranexamic acid good for sensitive skin?
In certain individuals with sensitive skin, topical tranexamic acid might be irritating.
- Is tranexamic acid prescription only?
There are low-potency forms of topical tranexamic acid creams and skincare products available without a prescription, but these are not very effective.
- Is tranexamic acid prescription only?
Treatment of melasma using tranexamic acid(TA) sometimes involves the use of a skincare cream that contains the TA. Generally, these creams are far less effective (and less concentrated) than injected, microneedled, or oral applications. However, tranexamic acid creams are available over-the-counter(OTC) without a prescription, making them affordable and accessible – if not all that effective.
- Does melasma come back after tranexamic acid?
The jury is still out on whether TA significantly reduces the recurrence of melasma after the course of the medication is completed. This is an area of active study in medicine. However, what we do know is that the recurrence rate is at least as good as in those not treated – meaning it doesn’t make you more likely to have a recurrence or flare afterward. Right now, we know short-term recurrence is around 1/3 of people with melasma in a 3-month period1, and there have been some small studies showing TXA can extend that when used in certain ways, but we need more data to say conclusively.
Good skincare and especially strict avoidance of sun exposure are suggested as well as year-round full spectrum sunblock. We know that avoiding sun exposure and limiting hormonal fluctuations are both very helpful in preventing future melasma patches.
- Will tranexamic acid work for my melasma? Who should not take tranexamic acid for melasma?
There’s no guarantee that tranexamic acid will work for you – and generally it has been thought of as a last resort of sorts for treating the melasma cases that are resistant to laser therapy and other medications, because it does have potential side effects, whereas laser therapy does not.
However, in one review of 560 melasma patients treated with tranexamic acid, 89.7% saw an improvement3. Of those, only 1 experienced a serious complication of deep vein thrombosis, and she was later found to have a rare disease.
Patients should not take tranexamic acid if they have a history of venous or arterial clots, actively smoke, or are taking oral contraceptive pills (birth control pills with hormones). Physicians at our practice review the medical history of the patient prior to prescribing the use of tranexamic acid, whether that’s topical or oral formulations because this drug is not safe for everyone to use.

Blog
How to Erase Your Summer Sins
Warmer weather may be coming to an end, but the effects of a summer well-spent...
Read More
Blog
Myth: Laser Treatment is for Light Skin Only
It is a popular misconception that cosmetic laser and light therapies are not...
Read MoreSources:
- Lajevardi, Vahideh, et al. “Comparison of the Therapeutic Efficacy and Safety of Combined Oral Tranexamic Acid and Topical Hydroquinone 4% Treatment vs. Topical Hydroquinone 4% Alone in Melasma: A Parallel-Group, Assessor- and Analyst-Blinded, Randomized Controlled Trial with a Short-Term Follow-Up.” Journal of Cosmetic Dermatology, vol. 16, no. 2, 2016, pp. 235–42. Crossref, doi:10.1111/jocd.12291.
- Saki, Nasrin, et al. “Comparing the Efficacy of Topical Hydroquinone 2 versus Intradermal Tranexamic Acid Microinjections in Treating Melasma: A Split-Face Controlled Trial.” Journal of Dermatological Treatment, vol. 29, no. 4, 2017, pp. 405–10. Crossref, doi:10.1080/09546634.2017.1392476.
- Lee, Hwee Chyen, et al. “Oral Tranexamic Acid (TA) in the Treatment of Melasma: A Retrospective Analysis.” Journal of the American Academy of Dermatology, vol. 75, no. 2, 2016, pp. 385–92. Crossref, doi:10.1016/j.jaad.2016.03.001.

Dr. Mitchell Chasin is a Cosmetic & Laser Physician at Reflections Center. Dr. Chasin believes strongly that the best cosmetic physicians are those who are dedicated to mastering their craft through continuing education and collaboration with the industry’s top doctors.